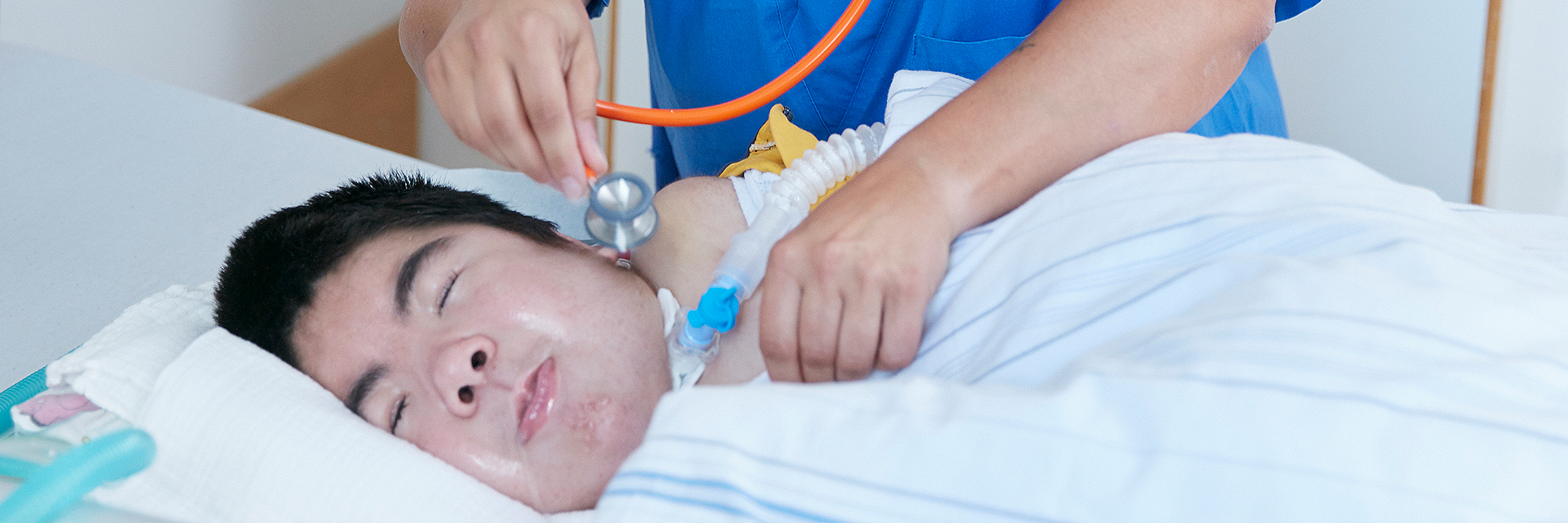
Respiratory therapy
Recognising and treating impaired respiratory function
Neurologically ill children and adolescents may have a restriction of respiratory function. We speak of a respiratory pump weakness when muscle weakness, reduced vigilance or even dysphagia with aspirations reach a critical level. Recognising and treating the corresponding symptoms is the task of our paediatric respiratory therapist together with the medical team.
Chronic respiratory pump weakness leads to insufficient gas exchange in the lungs. This so-called chronic hypoventilation often manifests itself at the beginning with sleep-related breathing disorders, restless sleep, nightmares. This can be accompanied by daytime sleepiness, headaches and weight loss. If left untreated, frequent respiratory infections and increasing signs of shortness of breath follow, even when awake.
There are a number of medical conditions that are regularly associated with hypoventilation. These include central respiratory regulation disorders (for example, diseases of the brainstem), neuromuscular diseases (including SMA, Duchenne muscular dystrophy, myotonic dystrophy), severe scoliosis and obstructive sleep apnoea/hypoventilation.
With our therapeutic interdisciplinary concept, we try to anticipate the course of the underlying disease with all possible complications as best as possible and to achieve, among other things, appropriate airway and secretion management.
In addition to the medical aspects, it is important for us to maintain the best possible quality of life and social participation of those affected and their families.
For the time after the hospital stay, respiratory therapy takes care of the transition and discharge management in cooperation with the social and medical services. Here we cooperate with outpatient nursing services and homecare supply teams and take care of prescriptions for medical equipment and materials. Another important area of responsibility of respiratory therapy is the training of relatives and the nursing staff.
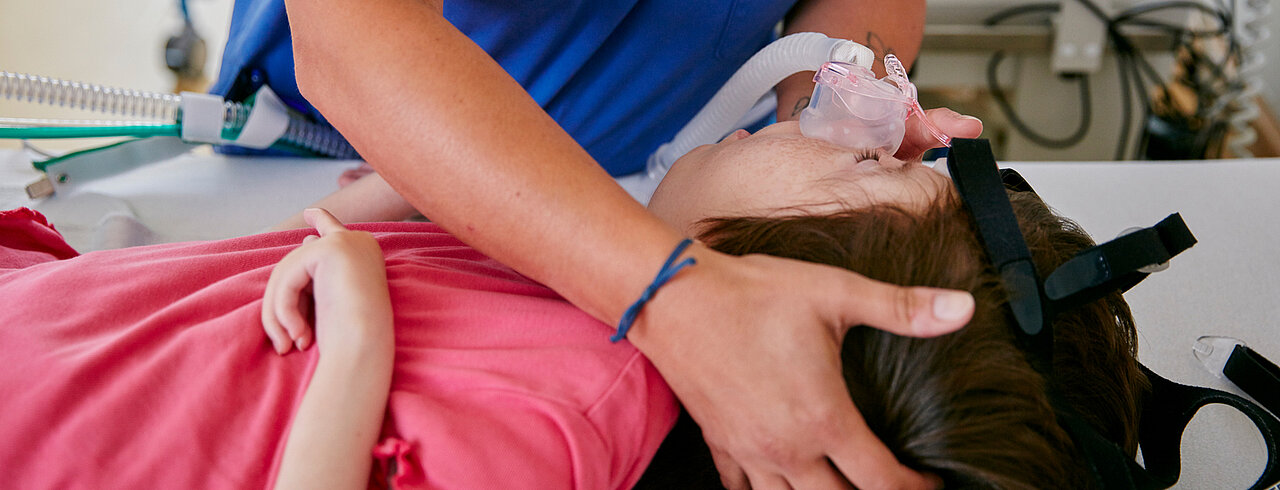
Relearn, improve, train breathing
Our respiratory therapy activities include not only recognising but also assessing the extent of respiratory pump weakness and initiating appropriate therapy.
It is important to regularly check the situation with a respiratory pump weakness, as it can worsen as well as improve. Accordingly, respiratory pauses or respiratory weaning can take place. If a tracheostoma is present, we establish an appropriate care concept for it. If it seems possible to dispense with the tracheostomy tube, we initiate and coordinate the necessary measures. Last but not least, we take care of secretion mobilisation and reduction.
Technical terms simply explained
If fluid, body secretions or food gets into the lower airways, i.e. into the windpipe or lower, there is aspiration. This usually triggers a cough reflex. If this is not the case, it is called "silent" aspiration. It can lead to aspiration-related pneumonia (aspiration pneumonia) particularly frequently.
The respiratory pump enables inhalation and exhalation and is thus the basis for gas exchange. Weakness of the respiratory pump can have many causes, for example muscle weakness, stiffening of the chest or reduced vigilance (see there). The term is often used to distinguish it from a problem with gas exchange, i.e. a lung problem.
Disturbance of the respiratory drive, e.g. if the respiratory centre is (also) affected by a disease.
Non-invasive ventilation (NIV) is a ventilation method that uses the upper airways (mouth, nose, throat). It has significant advantages and disadvantages compared to invasive ventilation.
Invasive ventilation, on the other hand, is done by bridging the mouth, nose and throat with a breathing tube and pushing it into the windpipe. This is usually not tolerated if consciousness is maintained. A special case is invasive ventilation via a tracheal cannula, which can also be tolerated by people who are conscious.
A few drops of blood are needed for this. The oxygen and carbon dioxide content, among other things, can then be measured in these. This allows a better assessment of the breathing situation or the ventilation situation than simply observing breathing and monitoring with a pulse oximeter.
A continuous positive air pressure is generated in the airways via a mask that is placed tightly over the mouth and nose (often only at night). This keeps the airways open and serves to avoid phases of insufficient air circulation in the airways or apnoea phases (lack of air circulation), as constantly occurs in the context of obstructive sleep apnoea syndrome (OSAS).
Breathing is used for gas exchange, i.e. to supply the body or the bloodstream with fresh oxygen in exchange for carbon dioxide. Gas exchange takes place in the alveoli (air sacs in the lungs).
Small ventilator, usually equipped with a rechargeable battery and thus functioning on the move, with which the -permanent or temporary- ventilation of a person can also be carried out outside an intensive care unit or a hospital by appropriately trained persons.
A machine administers a relatively large amount of air (with or without supplemental oxygen) into the patient's nasal vestibule through a tube for respiratory support.
This almost always refers to a progressive, i.e. continuously worsening, disease of muscles and/or nerves.
The obstruction of the airways during sleep leads to breathing pauses (see also CPAP ventilation).
Measures aimed at reducing mucus in the respiratory tract.
Curvature and often reduced mobility of the spine associated with it, can also make breathing difficult or restrict it.
A cannula ("tube piece"), usually made of plastic, adapted to the anatomy of a tracheostoma, i.e. a tracheal incision, and the trachea. It keeps the tracheotomy open and allows breathing bypassing the upper airway. Tracheal cannulae are available in many different sizes with many different additional functions, e.g. so-called "speaking cannulae".
an unnatural reduction in wakefulness and alertness, i.e. independent of tiredness or possible sleep.

